CortiCare Webinars
Insula – The Lesser Known Fifth Lobe
Insula- The Lesse Known Fifth Lobe Presented by Navita Kaushal PhD, REEGT, RNCST, CLTM Embedded deep beneath the sylvian/lateral fissure, pyramidal shaped covering less than 2% of the cortex, with […]
Watch NowTemporal Lobe Epilepsy

This webinar reviews the functions of the temporal lobe, seizure semiology and electrographic patterns of temporal lobe seizures. This webinar is an excellent review of the EEG patterns and semiology […]
Watch NowFrontal Lobe Epilepsy
This webinar reviews the functions of the frontal lobe, seizure semiology and electrographic patterns of frontal lobe seizures. The frontal lobe is the largest lobe and frontal lobe epilepsy is […]
Watch NowThe Future of Neurodiagnostics in the Age of ChatGPT

Presented by Dr. Allan Waziri, MD. With the release of ChatGPT to the general public the role and impact of Artificial Intelligent technologies is a hot topic. Healthcare has seen […]
Watch NowNormal Graphoelements of Neonatal EEG
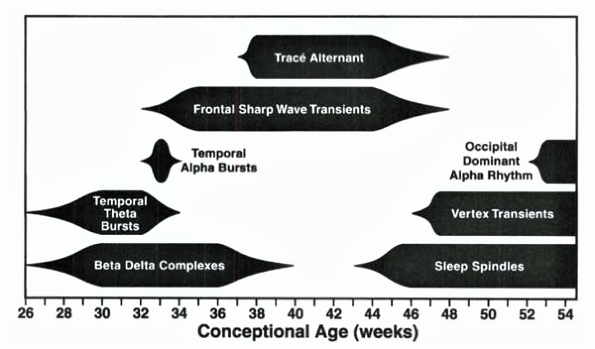
This webinar, presented by Dr. Audrey Nath, reviews elements of the neonatal EEG in both full-term and pre-term infants, including the neonatal montage, background features by gestational age, as well as […]
Watch NowSEEG and Semiology in the Study of Refractory Epilepsy
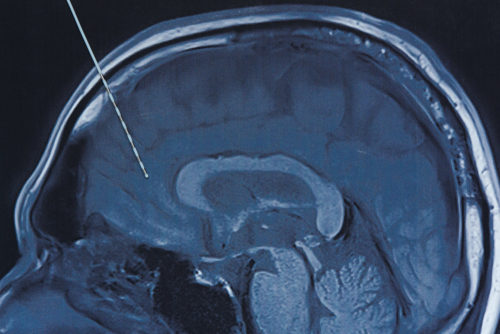
The use of Stereoelectroencephalography (SEEG) has rapidly increased over the last decade and there is growing interest in this method of intracranial EEG monitoring. This webinar reviews the basic principles of […]
Watch NowAn Update on EMUs and the NAEC Standards
The National Association of Epilepsy Centers (NAEC) has produced standards for the accreditation of epilepsy centers. In particular, “The Guidelines for Essential Services, Personnel, and Facilities in Specialized Epilepsy Centers […]
Watch NowCurrent Practice of Pediatric and Neonatal ICU EEG Monitoring
Guidelines for pediatric and neonatal ICU EEG monitoring are available to provide direction to pediatric epileptologists and neurocritical care physicians. However, the implementation of these guidelines and current practice varies […]
Watch NowUsing EEG for Subject Enrichment in Clinical Trials

Pharma clinical trials for new medications or other interventions that may impact or compromise brain function require that EEG be recorded, monitored, and analyzed. But EEG can also be a […]
Watch NowPNES: Not Everything That Shakes is a Seizure
Some patients exhibit behaviors that at first glance appear to be seizure related. However, there can be other causes and driving factors that result in these real symptoms and behaviors. Psychogenic non-epileptic […]
Watch Now